Hygiene is about preventing harm from infectious microbes or other harmful agents by preventing them transmitting to people, animals and products in numbers sufficient to cause harm.
Cleaning and disinfection have key roles in hygiene, but hygiene is founded on good working practices such as physical separation of clean and dirty items so that opportunities for cross-contamination and transmission are limited as far as possible at the outset.
Cleaning and disinfection are distinct but complementary processes. Cleaning is about the physical removal of dirt, including both microbes and the nutrients which can fuel the growth of bacteria and fungi for example. Disinfection is about ‘killing’ or inactivating germs and other harmful agents, whether by the chemical action of a disinfectant or antiseptic product or by physical means such as heat or UV light.
Modern hygiene systems seek to deliver and continuously assure good hygiene by analyzing risks, determining safe levels, defining procedures to achieve them and monitoring performance.
Physical separation
The foundation of good hygiene, which seeks to minimise opportunities for microbial cross-contamination throughout a process, is the physical separation of clean and dirty (contaminated) items and processes.
During food preparation, for example, raw and cooked food must be kept and handled separately. If they must sometimes occupy the same space, they should only be there at different times, with a suitable cleaning and disinfection process in between.
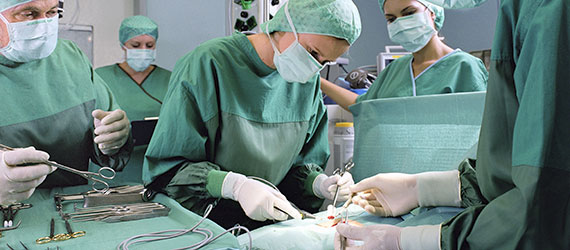
The same principle applies in other areas, such as operating theatres. There are either separate rooms for septic and aseptic surgery, or septic surgery is done at the end of the day followed by thorough disinfection of the whole theatre. Any item that is used in two consecutive processes, such as an endoscope, must be thoroughly decontaminated before the second use to avoid the transfer of microbes, in this case from one patient to another.
Cleaning
While separation of clean and dirty processes achieves a great deal, the risks of casual contamination of clean processes can be further minimized by regular cleaning and/or disinfection of the sources of that contamination – surrounding surfaces, items, equipment and instruments for example – and by frequent washing or disinfection of the most common means of transfer, the hands.
Cleaning and disinfection are only a part of hygiene, and products can only deliver their benefits within a properly managed framework of good practice.
A thorough cleaning step can remove around 99% of microbes from a surface, and higher removal rates are possible with advanced cleaning tools such as microfiber cloths. The microbes removed by cleaning are not usually killed, however, and unless they are efficiently rinsed away with clean water, they can contaminate the cleaning equipment and solution and be spread again when cleaning the next area.
Cleaning should be followed by thorough rinsing and drying, which also removes nutrients and moisture and inhibits survival and re-growth of any residual microbes.
Cleaning is often used as a first step prior to disinfection. Cleaning makes the microbes more accessible to the disinfectant, and removes dirt which can reduce its performance and undermine reliability. Some products are formulated to combine cleaning and disinfection capabilities and permit a single-step process for some applications.
Disinfection
Thorough cleaning can make many low-risk surfaces and items sufficiently free from microbes to pose little risk. But in many higher-risk situations, even a 99.9% reduction is far from enough to be safe. Microbe numbers on contaminated items are often measured in millions, and cleaning alone may leave thousands remaining. This is more than enough for some organisms to cause infection directly, and only a small number of organisms contaminating and growing in food, or entering the bloodstream, can cause major problems.
In such situations, microbial numbers must be further reduced by disinfection. This involves killing / inactivating microbes, and it can be achieved by chemical or by physical processes (e.g. using heat or UV light).
Though many substances will inactivate some kinds of microbes, national and international standards and test methods have been developed to determine whether a disinfectant has the appropriate efficacy for a particular application.
In some specific situations, such as for surgical instruments, safety demands complete elimination of all microbes, known as sterilisation. This may also be achieved by physical and /or chemical methods, including ‘autoclaving’ at high pressure.
Systematic approaches
Modern hygiene systems tailor packages of measures for each specific application that will work together to minimise the risks of transmission of infection, or of other adverse effects of microbes.
Professional hygiene begins with the identification of the potential risk factors for each situation. Using tools like HACCP and RABC, the relative importance of each hazard is assessed, and the critical steps to control the risks are identified. Hygiene systems are built upon sound working practices that seek to avoid opportunities for cross-contamination wherever possible. Cleaning and disinfection steps are then selectively built into this framework in a systematic and targeted way to control the remaining risks at critical places and times, and provide appropriate margins of reliability and safety.